Magnetic Resonance Cholangiopancreatography (MRCP)
- What is Magnetic Resonance Cholangiopancreatography (MRCP)?
- What are some common uses of the procedure?
- How should I prepare for the procedure?
- What does the equipment look like?
- How does the procedure work?
- How is the procedure performed?
- What will I experience during and after procedure?
- Who interprets the results and how do I get them?
- What are the benefits vs. risks?
- What are the limitations of MRCP?
What is Magnetic Resonance Cholangiopancreatography (MRCP)?
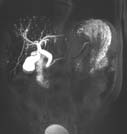
Magnetic resonance cholangiopancreatography (MRCP) is a special type of magnetic resonance imaging (MRI) exam that produces detailed images of the hepatobiliary and pancreatic systems, including the liver, gallbladder, bile ducts, pancreas and pancreatic duct.
Magnetic resonance imaging (MRI) is a noninvasive medical test that helps physicians diagnose and treat medical conditions.
MRI uses a powerful magnetic field, radio frequency pulses and a computer to produce detailed pictures of organs, soft tissues, bone and virtually all other internal body structures. The images can then be examined on a computer monitor, transmitted electronically, printed or copied to a CD. MRI does not use ionizing radiation (x-rays).
Detailed MR images allow physicians to evaluate various parts of the body and determine the presence of certain diseases.
What are some common uses of the procedure?
Physicians use MRCP to:
- examine diseases of the liver, gallbladder, bile ducts, pancreas and pancreatic duct. These may include tumors, stones, inflammation or infection.
- evaluate patients with pancreatitis to detect the underlying cause.
- help to diagnose unexplained abdominal pain.
- provide a less invasive alternative to endoscopic retrograde cholangiopancreatography (ERCP). ERCP is a diagnostic procedure that combines endoscopy, which uses an illuminated optical instrument to examine inside the body, with iodinated contrast injection and x-ray images.
How should I prepare?
You may be asked to wear a gown during the exam or you may be allowed to wear your own clothing if it is loose-fitting and has no metal fasteners.
Guidelines about eating and drinking before an MRI exam vary at different facilities. Usually, you will be instructed not eat or drink anything for several hours before your procedure.
Because your procedure may require use of a contrast material that is swallowed or injected into your bloodstream, the radiologist or technologist may ask if you have allergies of any kind, including allergies to food or drugs, hay fever, hives or allergic asthma. However, the contrast material used for an MRI exam is based on gadolinium and does not contain iodine. A gadolinium contrast agent is less likely to cause an allergic reaction compared to the iodinated contrast agents used in CT scanning.
The radiologist should also know if you have any serious health problems and what surgeries you have undergone. Some conditions, such as kidney disease, may prevent you from having an MRI with contrast material.
Women should always inform their physician or technologist if there is any possibility that they are pregnant. MRI has been used for scanning patients since the 1980s with no reports of any ill effects on pregnant women or their babies. However, because the baby will be in a strong magnetic field, pregnant women should not have this exam in the first trimester of pregnancy unless the potential benefit from the MRI exam is assumed to outweigh the potential risks. Pregnant women should not receive injections of contrast material except when absolutely necessary for medical treatment. See the Safety page (www.RadiologyInfo.org/en/safety/) for more information about pregnancy and MRI.
If you have claustrophobia (fear of enclosed spaces) or anxiety, you may want to ask your physician for a prescription for a mild sedative prior to the scheduled examination.
Jewelry and other accessories should be left at home if possible, or removed prior to the MRI scan. Because they can interfere with the magnetic field of the MRI unit, metal and electronic objects are not allowed in the exam room. These items include:
- jewelry, watches, credit cards and hearing aids, all of which can be damaged
- pins, hairpins, metal zippers and similar metallic items, which can distort MRI images
- removable dental work
- pens, pocket knives and eyeglasses
- body piercings
In most cases, an MRI exam is safe for patients with metal implants, except for a few types. People with the following implants cannot be scanned and should not enter the MRI scanning area unless explicitly instructed to do so by a radiologist or technologist who is aware of the presence of any of the following:
- cochlear (ear) implant
- some types of clips used on brain aneurysms
- some types of metal coils placed within blood vessels
You should tell the technologist if you have medical or electronic devices in your body, because they may interfere with the exam or potentially pose a risk, depending on their nature and the strength of the MRI magnet. Some implanted devices require a short period of time after placement (usually six weeks) before being safe for MRI examinations. Examples include but are not limited to:
- artificial heart valves
- implanted drug infusion ports
- implanted electronic device, including a cardiac defibrillator, pacemaker or retained leads.
- artificial limbs or metallic joint prostheses
- implanted nerve stimulators
- metal pins, screws, plates, stents or surgical staples
In general, metal objects used in orthopedic surgery pose no risk during MRI. However, a recently placed artificial joint may require the use of another imaging procedure. If there is any question of their presence, an x-ray may be taken to detect and identify any metal objects.
Patients who might have metal objects in certain parts of their bodies may also require an x-ray prior to an MRI. You should notify the technologist or radiologist of any shrapnel, bullets, or other pieces of metal which may be present in your body due to accidents. Foreign bodies near the eyes are particularly important. Dyes used in tattoos may contain iron and could heat up during MRI, but this is rarely a problem. Tooth fillings and braces usually are not affected by the magnetic field, but they may distort images of the facial area or brain, so the radiologist should be aware of them.
 Your child may need to be sedated in order to hold still adequately during the procedure. If this is the case, you will be given instructions for your child about not eating or drinking several hours prior to sedation and the examination. For the safety of your child during the sedation, it is important that you fully understand and follow any instructions that have been given. After the procedure there will be a recovery period from the sedation. Your child will be discharged when the nurses and physicians believe he/she is sufficiently awake to be safely sent home.
Your child may need to be sedated in order to hold still adequately during the procedure. If this is the case, you will be given instructions for your child about not eating or drinking several hours prior to sedation and the examination. For the safety of your child during the sedation, it is important that you fully understand and follow any instructions that have been given. After the procedure there will be a recovery period from the sedation. Your child will be discharged when the nurses and physicians believe he/she is sufficiently awake to be safely sent home.
What does the equipment look like?
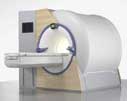
The traditional MRI unit is a large cylinder-shaped tube surrounded by a circular magnet. You will lie on a moveable examination table that slides into the center of the magnet.
Some MRI units, called short-bore systems, are designed so that the magnet does not completely surround you; others are open on the sides (open MRI). These units are especially helpful for examining patients who are fearful of being in a closed space and for those who are very obese. Newer open MRI units provide very high quality images for many types of exams; however, open MRI units with older magnets may not provide this same image quality. Certain types of exams cannot be performed using open MRI. For more information, consult your radiologist.
The computer workstation that processes the imaging information is located in a separate room from the scanner.
How does the procedure work?
Unlike conventional x-ray examinations and computed tomography (CT) scans, MRI does not depend on ionizing radiation. Instead, while in the magnet, radio waves redirect the axes of spinning protons, which are the nuclei of hydrogen atoms.
The magnetic field is produced by passing an electric current through wire coils in most MRI units. Other coils, located in the machine and in some cases, placed around the part of the body being imaged, send and receive radio waves, producing signals that are detected by the coils.
A computer then processes the signals and generates a series of images, each of which shows a thin slice of the body. The images can then be studied from different angles by the interpreting radiologist.
Frequently, the differentiation of abnormal (diseased) tissue from normal tissues is better with MRI than with other imaging modalities such as x-ray, CT and ultrasound.
How is the procedure performed?
MRI examinations may be performed on outpatients or inpatients.
You will be positioned on the moveable examination table. Straps and bolsters may be used to help you stay still and maintain the correct position during imaging.
Devices that contain coils capable of sending and receiving radio waves may be placed around or adjacent to the area of the body being studied.
If a contrast material will be used in the MRI exam, a physician, nurse or technologist will insert an intravenous (IV) catheter, also known as an IV line, into a vein in your hand or arm. A saline solution may be used. The solution will drip through the IV to prevent blockage of the IV catheter until the contrast material is injected.
You will be moved into the magnet of the MRI unit and the radiologist and technologist will leave the room while the MRI examination is performed.
If a contrast material is used during the examination, it will be injected into the intravenous line (IV) after an initial series of scans. Additional series of images will be taken during or following the injection.
The actual MRCP exam takes about 10 minutes, but it is often performed with a standard MRI of the abdomen, which may last approximately 30 minutes and involve the use of a contrast material. In this case, the entire examination is usually completed within 45 minutes.
What will I experience during and after the procedure?
Most MRI exams are painless. However, some patients find it uncomfortable to remain still during MR imaging. Others experience a sense of being closed-in (claustrophobia). Therefore, sedation can be arranged for those patients who anticipate anxiety, but fewer than one in 20 require medication.
If contrast material is used, there may be brief discomfort during initial placement of the intravenous catheter line.
It is normal for the area of your body being imaged to feel slightly warm, but if it bothers you, notify the radiologist or technologist. It is important that you remain perfectly still while the images are being obtained, which is typically only a few seconds to a few minutes at a time. You will know when images are being recorded because you will hear and feel loud tapping or thumping sounds when the coils that generate the radiofrequency pulses are activated. Some centers provide earplugs, while others use headphones to reduce the intensity of the sounds made by the MRI machine. You will be able to relax between imaging sequences, but will be asked to maintain your position without movement as much as possible.
You will usually be alone in the exam room during the MRI procedure. However, the technologist will be able to see, hear and speak with you at all times using a two-way intercom. Many MRI centers allow a friend or parent to stay in the room as long as they are also screened for safety in the magnetic environment.
 Children will be given appropriately sized earplugs or headphones during the exam. MRI scanners are air-conditioned and well-lit. Music may be played through the headphones to help you pass the time.
Children will be given appropriately sized earplugs or headphones during the exam. MRI scanners are air-conditioned and well-lit. Music may be played through the headphones to help you pass the time.
In some cases, intravenous injection of contrast material may be performed. The intravenous needle may cause you some discomfort when it is inserted and you may experience some bruising. There is also a very small chance of irritation of your skin at the site of the IV tube insertion. Some patients may sense a temporary metallic taste in their mouth after the contrast injection.
If you have not been sedated, no recovery period is necessary. You may resume your usual activities and normal diet immediately after the exam. On very rare occasions, a few patients experience side effects from the contrast material, including nausea and local pain. Similarly, patients are very rarely allergic to the contrast material and experience hives, itchy eyes or other reactions. If you experience allergic symptoms, notify the technologist. A radiologist or other physician will be available for immediate assistance.
Who interprets the results and how do I get them?
A radiologist, a physician specifically trained to supervise and interpret radiology examinations, will analyze the images and send a signed report to your primary care or referring physician, who will share the results with you.
What are the benefits vs. risks?
Benefits
- MRI is a noninvasive imaging technique that does not involve exposure to ionizing radiation.
- MR images of the soft-tissue structures of the body—such as the heart, liver and many other organs—are clearer and more detailed than with other imaging methods. This detail makes MRI an invaluable tool in early diagnosis and evaluation of cancer.
- MRI has proven valuable in diagnosing a broad range of conditions, including heart and vascular disease, stroke, and joint and musculoskeletal disorders.
- MRI can help physicians evaluate both the structure of an organ and how it is working.
- MRI enables the discovery of abnormalities that might be obscured by bone with other imaging methods.
- The contrast material used in MRI exams is less likely to produce an allergic reaction than the iodine-based contrast materials used for conventional x-rays and CT scanning.
- MRCP can produce images comparable to those obtained by a more invasive exam called endoscopic retrograde cholangiopancreatography (ERCP) without its associated risks including pancreatitis, or inflammation of the pancreas, perforation of pancreatic and bile ducts and bowel, and the risks for intravenous sedation required for ERCP.
Risks
- The MRI examination poses almost no risk to the average patient when appropriate safety guidelines are followed.
- If sedation is used, there are risks of excessive sedation. The technologist or nurse monitors your vital signs to minimize this risk.
- Although the strong magnetic field is not harmful in itself, implanted medical devices that contain metal may malfunction or cause problems during an MRI exam.
- There is a very slight risk of an allergic reaction if contrast material is injected. Such reactions usually are mild and easily controlled by medication. If you experience allergic symptoms, a radiologist or other physician will be available for immediate assistance.
- Nephrogenic systemic fibrosis is currently a recognized, but rare, complication of MRI believed to be caused by the injection of high doses of gadolinium-based contrast material in patients with very poor kidney function. Careful assessment of kidney function before considering a contrast injection minimizes the risk of this very rare complication.
- Manufacturers of intravenous contrast indicate mothers should not breastfeed their babies for 24-48 hours after contrast medium is given. However, both the American College of Radiology (ACR) and the European Society of Urogenital Radiology note that the available data suggest that it is safe to continue breastfeeding after receiving intravenous contrast. For further information please consult the ACR Manual on Contrast Media and its references. (www.acr.org/Quality-Safety/Resources/Contrast-Manual)
What are the limitations of MRCP?
High-quality images are assured only if you are able to remain perfectly still while the images are being recorded. If you are anxious, confused or in severe pain, you may find it difficult to lie still during imaging.
A person who is very large may not fit into the opening of certain types of MRI machines.
The presence of an implant or other metallic object sometimes makes it difficult to obtain clear images. Patient movement can have the same effect.
MRI generally is not recommended for patients who have been acutely injured; however, this is a clinical judgment. This is because traction devices and many types of life support equipment must be kept away from the area to be imaged. Furthermore, the examination takes longer than other imaging modalities (typically x-ray and CT) and the results may not be immediately available, as is often necessary in trauma situations.
Although there is no reason to believe that magnetic resonance imaging harms the fetus, pregnant women usually are advised not to have an MRI exam during the first trimester unless medically necessary.
MRI may not always distinguish whether edema fluid is caused by infection, inflammation or cancer. It generally cannot detect calcium present in soft tissues such as tumors.
Locate an ACR-accredited provider: To locate a medical imaging or radiation oncology provider in your community, you can search the ACR-accredited facilities database.
This website does not provide costs for exams. The costs for specific medical imaging tests and treatments vary widely across geographic regions. Many—but not all—imaging procedures are covered by insurance. Discuss the fees associated with your medical imaging procedure with your doctor and/or the medical facility staff to get a better understanding of the portions covered by insurance and the possible charges that you will incur.
Web page review process: This Web page is reviewed regularly by a physician with expertise in the medical area presented and is further reviewed by committees from the American College of Radiology (ACR) and the Radiological Society of North America (RSNA), comprising physicians with expertise in several radiologic areas.
Outside links: For the convenience of our users, RadiologyInfo.org provides links to relevant websites. RadiologyInfo.org, ACR and RSNA are not responsible for the content contained on the web pages found at these links.
Images: Images are shown for illustrative purposes. Do not attempt to draw conclusions or make diagnoses by comparing these images to other medical images, particularly your own. Only qualified physicians should interpret images; the radiologist is the physician expert trained in medical imaging.
This page was reviewed on May 02, 2013


 Pediatric-specific content
Pediatric-specific content 

